The Flexible Flatfoot in the Adults
The adult acquired flatfoot deformity is characterized by flattening
of the medial longitudinal arch with insufficiency of the supporting
posteromedial soft tissue structures of the ankle and hindfoot.
Aetiology
Although the etiology of this deformity can be arthritic
or traumatic in nature, it is most commonly associated with posterior tibial
tendon dysfunction (PTTD). Developmental etiologies also may be responsible for
a flexible flatfoot deformity. These include conditions associated with soft
tissue laxity (Ehlers-Danlos and Marfan syndromes), accessory navicular, and
neuro-muscular diseases. Extrinsic factors are less common but can result from
trauma involving the medial structures in an eversion type injury.
Two potential mechanical causes of an acquired flatfoot
deformity include medial column instability and a contracture of the Achilles
tendon or gastrocnemius fascia. With the former, medial column instability
results in forefoot varus and a compensatory hindfoot valgus. With the latter, a
tight Achilles tendon or gastrocnemius fascia results in transmission of dorsiflexion
forces from the ankle to the transverse tarsal joint and midfoot. This leads to
midfoot collapse and hindfoot valgus with lateral peritalar subluxation of the
navicular and subfibular impingement.
Pathology
An acquired flexible flatfoot deformity is most often associated with
Posterior Tibial tendon (PTT) dysfunction. Biomechanic overloading as described
above can lead to chronic microtrauma in the tendon.
With advancing age, the tendon’s elastic
compliance decreases because of changes in collagen structure, thus creating a
pathologic sequence where tendon weakening results in failure of the static stabilizers of the arch. Poor blood
supply may initiate this process or may prevent an adequate healing response,
resulting in chronic inflammation, tenosynovitis, and tendinosis.
Clinical Examination
Patients usually complain of medial ankle and hindfoot pain that
radiates to the arch of the foot or proximally to the leg. As the deformity
progresses, there may be a complaint of lateral or sinus tarsi pain caused by
subfibular impingement. Although some patients will attribute a nonspecific
traumatic event to the pain, most patients will relate a gradual onset of the
pain with loss of the medial plantar arch over recent months or years.
On physical examination, it is helpful to evaluate the
patient in short pants with both shoes off. This allows the clinician to note
the alignment of not only the foot and ankle, but also the knee. With genu
valgus, an individual’s center of gravity may be altered and more load may be
placed on the medial ankle and PTT. Comparison of tread wear on the shoes may
reveal more posteromedial wear than the opposite side. On examination of the
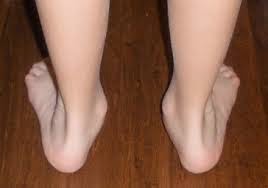
standing patient from behind, the presence of hindfoot valgus can be noted and
measured, and the “too many toes”
sign can be identified. The patient should be asked to perform a double leg heel rise so that the
presence or absence of hindfoot inversion can be identified. Next, the patient
is asked to perform a single leg heel
rise on the affected side noting that inability to do so is consistent with
PTTD.
Examination sitting should include assessment of ankle
and subtalar range of motion. Ankle motion should be measured with the knee
extended and flexed with the transverse tarsal joint locked and unlocked. This
will allow the examiner to assess for Achilles tendon and gastrocnemius
contractures. Palpation of the posteromedial ankle and hindfoot may reveal tenderness,
swelling, or fullness. The sinus tarsi, talar dome, and navicular tuberosity
should be palpated. Callus formation over the subluxated talar head may be
noted. For patients who have a flexible flatfoot, reduction of the
talonavicular joint and correction of the hindfoot valgus/forefoot abduction is
possible. Lastly, the PTT strength is tested with resistance against the inverted
and plantarflexed foot.
Diagnostic Imaging
Clinical examination and radiographs (in weight bearing Position) are
usually sufficient to establish the diagnosis of PTTD. In certain instances,
however, the use of MRI can be helpful to confirm the diagnosis, evaluate the
amount of pathology in the PTT and spring ligament complex, and detect bone
edema.
STAGES of PTTD
Stage I consists of painful synovitis of the tendon.
Nevertheless, tendon length and function are maintained so there is no
deformity.
Stage
II disease, there is progressive
tendon dysfunction and a flexible flatfoot deformity develops.
Stage
III involves a rigid deformity with
stiffness and often arthritis of the midfoot and hindfoot.
Stage IV consists of tibiotalar valgus, usually with associated
arthritic changes.
Conservative Treatment
The stage and progression of the flatfoot deformity will
generally determine the degree and duration of the conservative treatment. The
initial treatment of the adult flexible flatfoot deformity (stage II PTTD)
focuses on improving symptoms by decreasing the forces transmitted through the
posteromedial hindfoot. The patient should be encouraged to lose weight, modify
repetitive loading activities, and use supportive shoes.
(Eric Giza, MDa,*, Gerard Cush, MDb, Lew C. Schon, MD)


No comments:
Post a Comment